NEONATOLOGY ON THE WEB

|
The Baby Incubators on the "Pike."
A Study of the Care of Premature Infants in Incubator
Hospitals Erected for Show Purposes.
Part 6.
By John Zahorsky, M.D.,
St. Louis, Mo.
St. Louis Courier of Medicine 32(5):265-275,
May, 1905.
(Continued from page 219, April, 1905, Number).
|
The Quantity of Water Needed.
Before dismissing the general subject of feeding it is necessary
to point out that since the infants are kept constantly in a very
warm, and often dry air, evaporation of water is very rapid;
consequently, an additional quantity of water must be supplied,
especially during the first few days. The consequences of an
insufficient water supply will be studied under a different topic.
This water is best supplied by diluting the milk given with a 3 to 5
per cent sugar solution. Equal parts of mother's milk and the sugar
solution is a very good mixture with which to begin. An additional
supply of sterilized water can be given per rectum. It is well to try
to give as much water (including that given in the milk) as is
represented by one-sixth the body weight. Thus, if an infant weighing
1500 grams is given 65 cc. of milk on the second day, he should
receive sufficient water so that the total fluid is near 250 cc. By
doing this all tendency to inanition fever or other complications may
be avoided. If the milk has been diluted and this infant takes 130
cc. of liquid by the mouth, an additional 120 cc. must be given by
the rectum in two or three injections. It is unnecessary to state
that this water must be at a temperature of about 99°.
VI.
The Morbidity.
While we attempt to formulate general rules which will obviate all
evils, the rearing of premature infants is such a complex problem
that special pains must be taken in each individual to prevent
diseases and symptomatic disorders. The physician's work consists in
preventing these disorders and, if they arise in spite of care, in
alleviating them. The premature baby is most susceptible to a variety
of influences which only exceptionally impress the healthy baby born
at term; hence, their diseases require special study. Congenital
malformation need not be discussed here.
The functional derangements which need special study, since they
are most frequently connected with the mortality, may be classified
under four heads:
- The Respiration.
- The Temperature.
- The Digestion.
- The Nutrition.
What additional light has our study at the Baby Incubators on the
"Pike" thrown on these subjects?
Cyanosis, Apnea, Asphyxia.
The most formidable derangement of the respiratory function is the
failure to breath, or apnea, and is characterized by cyanosis of the
skin and mucous membrane. The appearance of severe cyanosis always
signifies that the infant does not make adequate respiratory efforts.
I will use the term apnea to signify absence of respiration due to
insufficient excitation of the respiratory nerve centers. Asphyxia is
more properly applied to those cases in which some obstruction to the
ingress of air exists. However, I do not wish here to enter on any
controversial points relative to the proper use of these terms. This
tendency to cyanosis depends partly on the atelectasis present, but
more especially on the feebleness of the respiratory muscles and,
above all, on the lessened irritability of the nerve centers.
Cyanosis is the principal cause of death among infants weighing
less than 1200 grams. All the infants under this weight, during my
service, died of a single or repeated attacks of cyanosis. This
derangement, then, merits the most careful attention.
It is astonishing what feeble respiratory movements on the part of
the infant is sufficient to insure an adequate supply of oxygen. When
these movements stop the infant which has a very red appearance
shows, after a few moments, a dusky red color, this gradually deepens
into a bluish red, dark blue and, finally, almost black color. If the
asphyxia persists pallor supervenes, which usually means death, that
is a failure of the heart also. What brings on these attacks after an
infant has breathed very well? Budin has very clearly laid this down
(Le Nourrisson, page 29).
Besides the reduction of temperature an insufficient quantity of
nourishment is given as a principal cause. Perrett also gives the
reduction of body temperature and insufficient alimentation as the
principal causes of cyanosis. Little else on this subject is to be
found in literature.
From the study of our records the etiological factors of cyanosis
appear to be many. In the first place the birth weight of the infant
has a marked influence. Infants weighing less than 1200 grams are
almost invariably attacked. So also a gestation of less than 28 weeks
seem to endow so little breathing capacity that cyanosis would almost
inevitably appear. Most infants do not die of one attack; very
commonly several attacks preceded death. Cyanosis, especially if the
attacks would be prolonged or frequently repeated, was invariably
accompanied by a reduction of the rectal temperature, even when the
baby was not removed from the incubator. The suspension of
respiration leads to a lessened tissue oxydation, and thus
predisposes to other attacks.
The next question to be answered is what relation has the rectal
temperature to the appearance of cyanosis? Budin gives the cooling of
the body as a cause, and no doubt he is correct. On the other hand,
it must not be forgotten that the cooling of the skin is one of the
most powerful stimulants to respiration (see Knapp, Scheintod der
Neugeborenen, for a discussion of this subject). Furthermore, an
elevation of temperature also endangers life by causing the
appearance of cyanosis. This is well exemplified by a series of cases
(First Series) in which the incubator was kept at a relatively high
temperature (94 to 98°). See the relation of the high
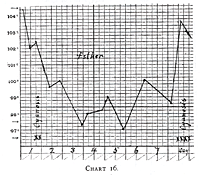
temperature and cyanosis in Charts 16 to 21. Especially in the case
of Esther (Chart 16) the cyanotic attacks indicated by the sign X,
were manifest only when the rectal temperature was over 102°.
Hence, an elevation of temperature over 102° predisposes to
cyanosis. This is another reason why the incubator should not be kept
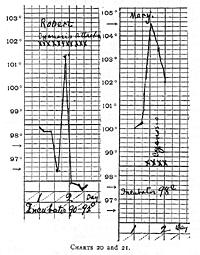
too high. But even when the temperature is perfectly normal (Chart
21), as in the case of Robert, repeated attacks of cyanosis may
appear.
An inquiry into the other direction is less definite. Many infants
weighing more than 1200 grams had a rectal temperature of 95.3°
without the appearance of cyanosis. Yet it can not be denied that
cyanosis is the dangerous symptom of too great loss of heat, but it
could not be determined at what temperature it is likely to appear.
Two infants who were admitted with a temperature of 93° did not
show this symptom. As in elevations of temperature it is often
impossible to decide whether it is the reduction in temperature or
the cause back of this reduction that is responsible for the
respiratory cessation. To be more specific, a few cases may be cited:
Case 43. -- Deaderick, gestation 24 weeks, weight 825
grams. Admitted with a rectal temperature of 93.4°. Placed in
incubator at 94 to 96°. Lived 18 hours. Rectal temperature never
exceeded 95.4°. Had three attacks of cyanosis.
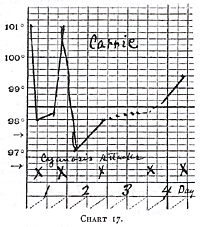
Care 48. -- W. K., gestation 24 weeks, weight 1100 grams.
Admitted with a temperature of 100°. Incubator temperature
90°. Rectal temperature dropped to 96° in nine hours, but
rose to 99° when the incubator was 92°; again dropped to
93° (incubator 90°), yet had no attack of cyanosis until
immediately before death, third day, with a rectal temperature of
96° (incubator 93°).
Case 51. -- C. K., gestation 28 weeks, weight 909 grams.
Admitted with a rectal temperature of 95°. Placed in incubator
at 93°. Rectal temperature the first day was between 94 and
96.4°. Third day became cyanotic with a rectal temperature of
97°.
It will be seen, therefore, that subnormal temperatures by no
means lead to repeated attacks of cyanosis. Altogether I can not
consider a rectal temperature of 96° very dangerous. A
temperature even below this does not mean an immediate attack of
apnea.
The respiratory movements, however feebly they seem, must be
relatively vigorous when there is much atelectasis, and to supply
this energy, food is necessary. Budin is undoubtedly correct in
assigning an inadequate food supply as a principal cause of cyanosis.
The infants, after a few hours or days, die from exhaustion, that
is, an insufficient fuel has reached the tissues and the respiratory
muscles and nerve centers give way first. In seven cases analyzed
from the First and Second series, that is, infants weighing less than
1200 grams, the food during the first forty-eight hours had an energy
quotient of less than 20 calories, and even part of this was rejected
by the stomach. To prevent cyanosis, then, the most careful attention
should be given to the food.
There is, however, one other danger, and that is overfeeding. Too
much food inevitably leads to indigestion and this to cyanosis. Thus,
in the baby Alice (Case 36, First Series), weight 1364 grams, the
energy quotient on the second day was 150 calories with indigestion
and repeated attacks of cyanosis resulting. Again, in that of Doris
(Case 38) the food quantity represented by an energy quotient of 140
calories on the first day resulted in death in two days, with the
temperature practically normal. Again, Henry (Case 42), on the
fourteenth day, with an energy quotient of 120 calories, but showing
marked dyspeptic symptoms had several attacks of cyanosis. With these
paroxysms the rectal temperature fell.
Cyanosis is also a symptom of inanition fever, or more properly, a
disturbance caused by an insufficient supply of water. In the infants
Pearl, Margaret, etc. (Cases 53-56), in addition to diluting the
milk, rectal injections of a physiologic salt solution were resorted
to in order to supply the necessary water. As mentioned previously,
the rapid evaporation in such superheated air (88-94°) must
always be considered, and careful attention to the rules laid down
for the administration of water will often prevent cyanosis.
While food is absolutely necessary to prevent cyanosis, it can not
be denied that the act of feeding in infants weighing less than 1200
grams is one of the principal causes of cyanosis. Paradoxical as it
may seem, feeding is dangerous to these infants. Most of the attacks
of cyanosis arise during or immediately after feeding. In the first
place, the very act of deglutition in certain infants will in some
way stop the respirations. I have noticed this particularly even
before this experience. Then again, a few drops of milk may lodge in
the mouth and incite no deglutition but stop the breathing.
The milk may enter the larynx during deglutition or from vomiting
afterward. If the head of the infant is kept down, as is often done
to increase the blood supply in the brain, and the infant is fed, the
milk may run into the nasopharynx and occlude the respiratory tube,
resulting in cyanosis.
During vomiting, also, the food often regurgitates through the
nose and fatal cyanosis may follow. Vomiting is very dangerous in
these feeble infants. I may better illustrate the difficulties and
dangers by reciting an experience:
Robert, weight 1000 grams, gestation 26 weeks, arrived with a
rectal temperature of 98.8°. While being dressed for the
incubator his first cyanotic attack appeared, which was relieved by
oxygen inhalations and artificial respiration. In spite of his
temperature being near normal constantly, and even above normal, with
nearly every feeding cyanosis would become manifest. For the first
nine hours nothing was fed except a few drams of 3 per cent. sugar
solution. This feeding was certainly inadequate. It is necessary to
begin feeding as soon as possible. In the following twenty-four hours
food representing an energy quotient of 24 calories was administered
but much of this was not retained.
After twelve hours' trial of feeding with a dropper, gavage was
resorted to, with no change as to the number of attacks of cyanosis.
Vomiting was frequent after gavage, many times the milk was
regurgitated through the nose. Altogether he was a promising baby and
yet in spite of the most careful work for two days, the cyanotic
attacks did not diminish (Chart 20).
In this little patient, the fact was demonstrated that even with
the best of care, infants of not more than 26 or 28 weeks' gestation
and weighing less than 1200 grams, life will become extinct.
Finally, fatal attacks of cyanosis, with or without a rise of
temperature, occurring after the second day, indicates a local or
general infection. This may occur in any premature infants (Chart
16). The history of one case will suffice:
Case 45. -- E. H., male, gestation 7 months, weight 1930
grams. Admitted, after a ride of seven miles over rough roads, in
fair condition. He had two attacks of cyanosis on the way. Rectal
temperature, on admission, 102.6°. Placed in the incubator at a
temperature of 88°. Rectal temperature on the first day 98 to
100°, second day 99 to 101.2°. On the afternoon of the
third day the temperature suddenly rose to 102.8°. Small
cutaneous hemorrhages appeared in various parts of the body.
Diagnosis: Hemorrhagic disease caused by some infection.
Food supply, mother's milk in quantities of 4 cc. every hour,
increased to 6 and 8 cc. The alimentation gave the following energy
quotient: First day, 30 calories; second day, 35 calories; third day,
40 calories. Additional water was given by the rectum after the
second day. A slight attack of cyanosis occurred on the evening of
the second day, with a temperature of 100°. Twice on the
following morning the infant became blue, with a rectal temperature
of 100.2°. In the morning of the third day the rectal
temperature rose to 102.8°, and frequent attacks of cyanosis
ended fatally.
Many additional cases could be cited from the First Series, but
this will illustrate the statement that fatal cyanosis occurs on
account of an infection.
The treatment of cyanosis is to ascertain the cause and remove it.
For the attacks, artificial respiration takes first place. During
feeding the nurse must watch the breathing and if the slightest
cyanosis appears, must stop the feeding and restore the breathing.
Pinching the baby often restores this function. Tapping on the head
with the finger will remind the nervous system to act. When these
methods are insufficient, artificial respiration, to initiate the
respiratory function, must be employed. Before doing this one must be
sure that the upper respiratory tube is clear of milk or mucus. The
baby is rolled on its face and the head lowered. Milk will then flow
out of the larynx or pharynx. It can then be wiped away.
As to the method of artificial respiration, the exigencies of the
case must decide. Undoubtedly, Schultze's method is the most
effective, but has the great objection that swinging rapidly cools
the infant. If the rectal temperature is high, this method can be
used. When the temperature is subnormal other methods should be
chosen. Marshall Hall's method is applicable in the incubator.
Silvester's method will more generally be found serviceable and can
be used in the incubator or the bath. The infant should at once be
placed in a warm bath (temperature 100° F.) if the rectal
temperature is below 36° C.
It is well to have several methods of artificial respiration in
mind, as different conditions necessitate the choice of different
procedures. The methods of Pacini, Bain or Behm can be used in the
incubator. Prochownick's method (suspension by the feet and
compression of the chest) can be used advantageously if the cessation
of the respiration is caused by milk or mucus in the upper
respiratory tube. The method of Harvie does not necessitate exposure
so much as Schultze's procedure.
Simple suspension alone will often initiate respiration. The
method of Laborde was used in one case unsuccessfully.
One or two attempts at blowing air into the trachea were
unsuccessful. It was our custom in many cases to place one drop of a
1/1000 solution of nitroglycerin on the tongue of these babies. Often
it seems very helpful. Oxygen inhalations were constantly used. I am
not very sure as to its value. Oxygen can not initiate the
respiratory function. When the breathing has started, oxygen hastens
the oxygenation of the blood and dispels cyanosis.
Altogether the problem of cyanosis is one of the principal tasks
awaiting solution. With skill and great care its dangers may be
obviated, but in infants weighing less than 1200 grams, it is only
rarely that cyanosis will not appear.
Figures
|
|
Chart 16.
|
|
|
Chart 17.
|
|
|
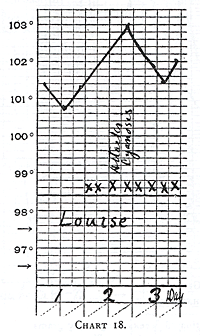
Chart 18.
|
|
|
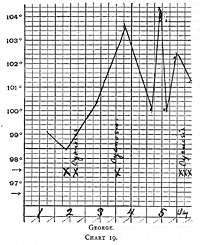
Chart 19.
|
|
|
Charts 20 and 21.
|
(To be Continued.)
Return to the Contents Page
Created 6/17/2000 / Last modified 7/16/2020
Copyright © 2000-2020 Neonatology on the Web / webmaster@neonatology.net





