Neonatal Blood Gas Testing
The development of blood gas testing for newborns is a story driven by a critical technological challenge: how to accurately monitor a critically ill infant’s respiratory and metabolic status without draining their highly limited blood supply. In premature infants, frequent traditional blood draws can quickly lead to iatrogenic (medically induced) anemia, sometimes necessitating blood transfusions.
In the 1950s, the foundation for modern blood gas analysis was laid with the invention of specific electrodes to measure oxygen (Clark electrode) and carbon dioxide (Severinghaus electrode), alongside pH meters. Danish physician Poul Astrup developed early clinical blood gas equipment during the polio epidemics to monitor patients’ breathing. These early benchtop machines were revolutionary but required several milliliters of arterial blood. For a premature baby whose total blood volume might only be 80–100 milliliters, taking 2–3 milliliters multiple times a day was extremely dangerous.

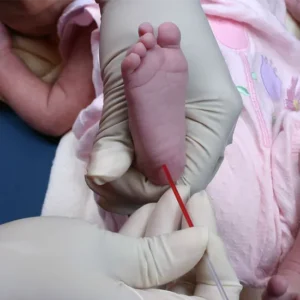
The 1960s saw the first major pivot toward conserving neonatal blood, pioneered largely by Astrup’s colleague, Ole Siggaard-Andersen. Researchers discovered that by warming a newborn’s heel to “arterialize” the capillary bed, they could obtain blood that closely mirrored arterial pH and pCO2 levels. Siggaard-Andersen developed micro-methods that allowed for pH and gas analysis using tiny capillary tubes. This reduced the required sample size from milliliters to about 50–100 microliters (muL), a massive leap forward for neonatology.
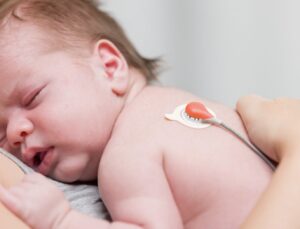
While not a blood test per se, the development of non-invasive monitors was the next major leap in reducing the need for blood draws altogether. During the 1970s, transcutaneous monitoring became available: electrodes were developed that could be heated and attached directly to a newborn’s skin to measure oxygen (tcPO2) and carbon dioxide (tcPCO2) diffusing through the skin. This was a welcome development: it reduced the need for blood draws, it allowed continuous monitoring, and it reduced pain and stimulation for the baby. Transcutaneous monitoring did have its drawbacks, however, it was finicky and labor-intensive because the location of the electrodes had to be changed frequently to avoid burning the baby’s skin.
The widespread adoption of the pulse oximeter in the 1980s allowed continuous, real-time tracking of oxygen saturation without a single needle stick. Blood gas tests were now only needed for periodic calibration or comprehensive metabolic checks (like pH and base excess), drastically reducing the frequency of draws. See the separate article on pulse oximetry for more details.
The most recent evolution in blood gas technology has been the use of biosensors and microfluidics to miniaturize the analyzers themselves, bringing testing directly to the bedside (Point-of-Care or POC testing). Modern technology has replaced bulky benchtop electrodes with single-use, microfabricated sensor cards. Systems like the i-STAT or modern Radiometer and GEM analyzers require incredibly small amounts of blood—often between 35 to 95 microliters (just a few drops). Despite the microscopic sample size, these modern cartridges can simultaneously measure pH, pCO2, pO2, electrolytes, lactate, and hemoglobin in roughly 60 seconds.



Left to right: Radiometer, GEM, and i-STAT Point-of-Care blood gas analyzers ca. 2026
In short, the technology of neonatal blood gas testing has evolved from milliliters in syringes required by bulky 1950s lab machines to capillary tubes holding microliters of blood drawn via heel-sticks in the 1960s, supplemented by zero-volume continuous skin monitors and pulse oximeters in the 70s and 80s, culminating in today’s bedside microfluidic cartridges that test a dozen parameters off a single drop of blood.
Timeline of Neonatal Blood Gas Testing Technology
| Decade | Key Technological Development | Clinical Impact & Sample Size |
| 1950s | Benchtop Electrodes: Invention of Clark (pO2) and Severinghaus (pCO2) electrodes. First commercial blood gas analyzers (Astrup). | Required multiple milliliters of arterial blood; high risk of medically induced anemia in premature infants. |
| 1960s | Micro-Methods & CBG: Introduction of Capillary Blood Gas testing via warmed heel-sticks. | Sample size drastically reduced to 50–100 µL, making routine metabolic monitoring much safer. |
| 1970s | Transcutaneous Monitoring: Heated skin electrodes developed for non-invasive tcPCO2 and tcPO2 tracking. | Introduced continuous, zero-volume monitoring between physical blood draws. |
| 1980s | Pulse Oximetry: Widespread adoption of real-time oxygen saturation monitoring in NICUs. | Drastically reduced the frequency of needle sticks, reserving them primarily for metabolic checks or calibration. |
| 1990s–Present | Microfluidics & POC Testing: Miniaturization of electrodes into handheld, bedside Point-of-Care cartridges. | Comprehensive panels (gases, electrolytes, hematocrit) run in 60 seconds on a single 35–95 µL drop of blood. |
Further reading on blood gas technology:
- Ball CM, Featherstone PJ: :Measurement of Blood Gases,” Anaesthesia and Intensive Care 50(4):270-272, 2022. https://journals.sagepub.com/doi/10.1177/0310057X221094741
- Severinghaus JW, Astrup P, Murray JF: “Blood Gas Analysis and Critical Care Medicine,” American Journal of Respiratory Critical Care Medicine 157:S114-S122, 1998. https://www.atsjournals.org/doi/10.1164/ajrccm.157.4.nhlb1-9
Last Updated on 02/25/26