Retrolental Fibroplasia: A Modern Parable – Chapter 12
Chapter 12
Progress in a Groove
Perinatal medicine has sprouted and grown rapidly in the past 25 years. The same period has been marked by a gradual (and overall) erosion in public trust of the medical profession and its institutions. I do not wish to imply that there is a simple cause-and-effect relationship between these two developments, but I find it hard to ignore the fact that the new field of medical activity has been singled out for special criticism by community groups in the United States and in Great Britain. I believe, therefore, that it may be useful to attempt to trace the roots of community versus profession conflict. The areas I will explore in this chapter are the narrowness of outlook which results from the atomistic approach to complex problems, the demographic and social consequences of medical actions, clash of values, and a communication gap between community and profession.
Modern attempts to acquire a mechanistic understanding of outstanding medical problems (in terms of physiology and biochemistry) have taken the only route possible: the path of reductionism. A complex system must be broken down into manageable segments, and the isolated parts examined in depth. Nonetheless, the dissection approach to problem-solving is the beginning, not the end, of a search for solutions. The dangers of the present-day situation were recognized many years ago by Whitehead:
. . . a great fact confronting the modern world is the discovery of the method of training professionals, who specialize in particular regions of thought and thereby add to the sum of knowledge within their respective limitations of subject . . . this situation has its dangers. It produces minds in a groove. Each profession makes progress, but it is progress in its own groove . . . Thus, in the modern world, the celibacy of the medieval learned class has been replaced by the celibacy of the intellect which is divorced from the concrete contemplation of the complete facts . . . The dangers arising from this aspect of professionalism are great, particularly in our democratic societies. The directive force of reason is weakened . . . In short, the specialized functions of the community are performed better and more progressively, but the generalized direction lacks vision. The progressiveness in detail only adds to the danger produced by the feebleness of coordination . . .
I believe that much of the public apprehension about modern perinatal medicine has come about as a result of uncoordinated advance “in detail.” As the intensity of activities has increased, what seems to have been ignored is that human infants are complex natural systems-they are wholes with irreducible parts. Errors, misconceptions and disharmonies have crept in as the focus of medical interest has narrowed to isolated biologic effects (unrelated to the interconnected physico-chemical “systems” of the infant organism) or to infants viewed out of context (as disconnected from intergrated social “systems” of the family, cultural group and community).
The profession should not be blamed for failing to foresee the unknown pathologic effect of supplemental oxygen on immature retinal blood vessels. But, it must be criticized, I believe, for its failure to expect the unexpected in the face of limitations of knowledge-to look beyond the immediate outcome of interest (breathing pattern). And, this dereliction occurred over and over with changes in feeding practices, administration of new drugs, expansion of facilities, and proliferation of equipment. The dangers of a narrow outlook are not confined to this field of medicine, but the lessons are particularly revealing because the hazards are exaggerated in the case of the fetus and newborn. In a figurative sense, these unknowing patients have served a function which is like that provided by a miner’s canary: they have given early warning of the danger of increasing hazards in medicine. The immature baby is a unique “species” of human being; he exhibits an unusual vulnerability to minor changes in the chemical and physical environment. For example, even the simple act of removing the clothes of a premature infant in a warm-air, transparent incubator had a major unexpected consequence. The focus of interest on observations of the baby’s respirations distracted attention away from the effect on heat balance: there was a net loss of body heat through radiant exchange between the warm naked skin surface and the relatively cool Plexiglass walls of the incubator. The importance of this subtle physical effect was completely overlooked for years. Persistently low body temperature, under conditions of warm incubator-air temperature, was considered to be a “characteristic of prematurity” (newborn infants, unlike older individuals, do not shiver when body heat is lost). Finally, in 1958, a formal trial was conducted which demonstrated that during the first days of life, surprisingly small differences in body temperature were associated with vital effects: small newborn babies survived in increased numbers when heat dissipation via the radiant route of heat loss was compensated by increased warmth to bring body temperature up. These results were confirmed and, since the 1960s, an enormous amount of information has been collected concerning temperature regulation in the period immediately after birth. Many other perinatal phenomena are now reasonably well understood, but, compared to the pond of knowledge, our ignorance remains Atlantic. Ironically, it is the confidence in a firm foundation of evidence in isolated biologic effects which tends to encourage the daring jump to widespread everyday applications. All of the time and effort involved in working out the details of specific physiologic mechanisms under carefully regulated conditions make the slow (and, by contrast, crude) steps of formal evaluation at the bedside seem like annoying roadblocks which have been put up to retard progress. And, as therapeutic exuberance has increased, the dangers arising from the tunnel vision of the impatient specialist are greater now than ever.
In addition to effects on infants as individuals, there are some demographic consequences of perinatal actions which are of public concern. In the United States, the most common conditions associated with infant deaths are prematurity (and its complications) and congenital malformations. After the age of 40, heart disease, malignancies, and strokes account for more than half of all deaths. Efforts to prolong life in these two periods (before and after the years of procreation) produce population impacts which are quite unequal. The reverberations of actions taken in nurseries are greater by far than those taken in adult sections of hospitals. The asymmetry has been true in the past and the preeminent importance to the community of the outcomes of pregnancy will undoubtedly persist. The demographic effects are both quantitative and qualitative.
The steady increase in life expectancy in the United States since the beginning of this century has been due primarily to the fall in mortality rates during early infancy and childhood. Since 1900, the expected duration of life for an infant has increased by approximately 22 years, while the life expectancy for an American of 40 has lengthened by only 6 years. Infant mortality in 1976 (15.1 deaths under 1 year of age per 1000 live births in the U.S.) was less than one-sixth of the rate 60 years earlier, and the decline in that year alone was the largest proportional drop in 20 years. Three-quarters of the deaths under 1 year take place in the first month after birth, and half of the infant deaths occur in the first 24 hours following delivery. Even small changes in the mortality rates at these early ages are reflected in large effects on present-day age distributions and on population size, and the effects are magnified in future generations: the rate of numerical increase in population is determined primarily by the numbers of children who reach the childbearing ages. Prolongation of life after the reproductive years has a relatively small and, of course, short term effect on total numbers of the population.
It is the survival of girls which tends to dominate effects on reproductive pressures and, thus, future population size. Harris has pointed out that this “explains” the frequent use of female infanticide as a population control measure in primitive societies who have no other means to balance the number of mouths to feed and the means of subsistence. For example, the number of births “expected” in a group of ten men and ten women would be the same as in a group consisting of one man and ten women. But, in a local group of ten men and only one woman, the birth rate “expected” would be one-tenth of the two other examples. All other things being equal, it is the number of women which determines the rate of reproduction. The sex composition of a population depends largely on the sex ratio among live born infants and the relative sex-specific mortality rates. As a result, it is of some interest to note that there are substantial differentials in the mortality of the sexes in infancy, particularly in the newborn period. More male infants are born (1054 males per 1000 females in the U.S. in 1975) but the disparity in numbers is quickly eroded by a striking excess of male mortality rates: the risk-margin in favor of girls is greatest in the first days and months; by 9-11 months of age the excess mortality among males narrows to 11 percent (Fig. 12-1). Mortality-risk for boys is greater than for girls at most birth weights (Fig. 12-2). The point to be made here is that the effect of reduction in early deaths (especially of small babies) is one of augmenting the ratio of females over males in the population. [For example, as infant mortality in the United States fell from the years 1940 to 1970, the percent excess of male over female mortality rates increased progressively (Table 12-1)]. A complex of effects may be felt in future generations, I suggest, as the result of present declines in birth rate and in perinatal mortality; age composition, sex ratio, and population size can be expected to be altered. My view of the potential effects of current medical activities (although the exact contributions of many specific actions have not been demonstrated, see Chapter 11) differs from McKeown’s conclusion concerning influences in the past. He found that medical measures have had relatively little effect on historical trends. The exponential rise of world population since the 18th century can be accounted for, in large part, by a fall in infant mortality. A main restraint on population growth before this time, McKeown observed, was the high level of deaths brought about by the limited capacity of the environment (particularly the availability of food) to support the number of babies born. He collected evidence which indicated that medical conquest of disease played a minor role in the modern rise of population, and that the level of fertility remained unchanged over this period. Obviously, the situation is changing dramatically. As environmental limiting effects decline and technical control of fertility and of perinatal mortality become more efficient, the levers which manipulate population numbers are (for the first time, if McKeown’s reading of history is correct) passing into medical hands.
The qualitative changes in demography resulting from intensified perinatal actions are difficult to measure. But information about genetic disorders gives some clue about biologic changes which may be expected as perinatal mortality falls. For example, about 40 percent of conceptions end in spontaneous miscarriage; a little more than half of these occur so early that a woman may not know that she is pregnant. Major chromosomal abnormalities are a leading cause of this substantial toll of fetal life. Serious genetic defects are present in about 4 percent of all live-born infants; the rate increases progressively with decreasing maturity and birth weight (the proportion is particularly high in infants who are undergrown, i.e., birth weight lower than expected for duration of pregnancy). Malformations are also a leading cause of death in the first days after birth and in infancy. Erbe notes that birth defects claim as many “life years” as does heart disease, eight times as many as cancer, and ten times as many as stroke. Thus, even a minor change in the survival of fetuses and infants with birth defects has a major demographic impact. In 1977, it was estimated that 12 million Americans have genetically caused birth defects. About 20-30 percent of all hospital admissions of children are related primarily to genetic disorders, and it is estimated that malformations are the commonest cause for hospitalization of children in North America. The net effect on these statistics of genetic screening programs during pregnancy, therapeutic abortion for identified genetic disorders, and falling perinatal mortality rates has not been calculated. And again, one can only guess about the effect projected to future generations which will result from the prolongation of life of children with serious heritable abnormalities. Consider, for example, the puzzles which are involved in cystic fibrosis. It is the most common, serious, recessively inherited disorder in the white population of the United States: it occurs in about one in 2000 births. The abnormality cannot, as yet, be diagnosed prenatally, and carriers (about 1/20 of the white population) cannot be identified. In the past, cystic fibrosis was considered to be uniformly fatal in infancy, many affected infants died soon after birth (often as the result of meconium ileus). Improvements in treatment have resulted in a steady increase in life-expectancy; the average age of survival was 15 years in 1970 and is now probably higher. From the community’s point of view, the costs and benefits of medical efforts in cystic fibrosis can be computed by using relatively uncomplicated economic weightings. But the biologic issues involved in working through the full consequences of medical policies for meconium ileus (and in other severe genetic disorders which are evident at birth) are enormously complex. And they cannot be dismissed by the phrase “of academic interest only.”
Table 12-1
Infant Mortality and Percent Excess of Male
Mortality Rates By Years (United States 1940-1970)
| Year* | All Infants | Males | Females | Percent Excess of Male Mortality |
| 1940 | 47.01 | 52.5** | 41.31 | 27.1 |
| 1950 | 29.2 | 32.8 | 25.5 | 28.6 |
| 1960 | 26.0 | 29.3 | 22.6 | 29.6 |
| 1970 | 20.4 | 23.3 | 17.5 | 33.1 |
| * Live-birth sex ratio remained unchanged over this period: 1055 males per 1000 female live-births in 1940, exactly the same ratio in 1970. | ||||
| ** Deaths under 1 year of age per 1000 live births. | ||||
I do not find it surprising that the difficult dilemmas posed by developments in perinatal medicine have been greeted with widespread apprehension in this country. Moreover, it is concern about drawing the line in the rescue efforts which has acted as a wedge in widening the gap of disagreement between the community and the medical profession. Chargaff has pointed to an unfortunate tendency which he associates with the current revulsion from science: we have begun to believe that the fact that something can be done carries its own justification. He terms this the “devil’s doctrine”: what can be done must be done. As noted above, the disharmony is not confined to the United States. In 1974, for example, a consumer group in England found more adverse comments about maternity services than any other branch of medical practice. Chalmers noted with interest that this criticism surfaced in Oxford, a city which had attained one of the lowest perinatal mortality rates in the United Kingdom. Even in developing countries with high rates of perinatal loss, the new childbirth technology has received a mixed reception. Medical staffs of health ministries strive to improve coverage of overall health services, rather than investment in expensive technology which benefits relatively few patients. But administrators lack the charisma of intensive-care specialists. The voice of caution has often gone unheeded. However, there is some evidence of general disillusion with high-cost, high-technology medicine which operates only within a relatively sophisticated environment. In many countries, the value of intensive technologic approaches has been seriously questioned when measured in terms of their impact on improving the health status of the populations. An article in the Bangladesh Times (Jan. 14, 1977) is revealing. The commentator called attention to an example of advice from western consultants which was completely unrealistic for his people and the environment: a laparoscope was recommended for every rural health center in Bangladesh. This highly sensitive, sophisticated instrument requires both electricity and gas to function; not all hospitals in Britain have a laparoscope, the reporter exclaimed. The same article also told of a discussion between the reporter and a friend from abroad. The visitor said that he had encountered 72 foreign advisors in Dacca on that day alone. “And yourself?”, the writer asked. “Seventy-three,” was the admission. The newsman concluded that it will be an uphill road, overcoming this favorable bias toward the wisdom of the west. Such an effort was made in 1974 at a workshop arranged by the West African Health Secretariat and convened in Ghana. The members of the workshop from five African nations recommended that highly trained doctors will have to consider accepting constraints on some activities hitherto regarded as sacrosanct. Lewis Mumford came to a similar conclusion in another, not entirely dissimilar, context. In 1946 he reviewed the crisis brought on by the advent of the nuclear age; he outlined a program for survival and pleaded that we do not forget the most essential secret of humankind’s advance; the practice of restraint.
What are the social effects of medical efforts to rescue fetuses and newborn infants? As I have indicated, the operations are more than technical achievements to be measured by vital statistics. They are social actions with powerful long-term effects on individuals. And, it is in the consequences of technical actions as seen in persons-taken one by one-that the “danger produced by the feebleness of coordination” is particularly high. The experience with RLF is illustrative of the failed opportunities to go beyond the limitations of an organ-bound perspective. For example, the huge 1953-54 Cooperative Study of RLF (as a condition affecting the eye) was disbanded after a year. But, the full expression of the chronic condition know as RLF-blindness (affecting the whole child, the family, social agencies, schools and community) was just beginning. In the past few years, I have contacted RLF-blinded young adults and, later, some of the parents to ask about their life experiences. I was surprised to learn that the young men and women (in their twenties) had only vague information about RLF and theories about the mechanism of the oxygen effect. Very few knew any details of the epidemic or about the national efforts to study the disorder and to control the outbreak. Many told me they had been puzzled for years; their parents and physicians seemed restrained by what the young people felt was a conspiracy of silence about the entire subject. I organized several small groups for informal marathon discussions. I told them everything I knew about the history and the medical aspects of the disorder; they told me what it was like to grow up without vision in the United States. I learned very quickly that loss of sight is not the major burden faced by blind children and young adults. Preconceptions, paternalism and insensitivity of authorities in the visually oriented world constrict the lives of those who wish to see this same world nonvisually.
Discussions with parents, singly and in groups, were much more difficult for me (and for them). Most of the parents were still bitterly angry at the medical profession, but not for the reason I imagined. They understood and accepted the fact of limited knowledge at the time their children were born. Most were convinced that physicians had rendered excellent care and had used supplemental oxygen liberally in well-meant efforts to improve the chances of the small babies for intact survival. But, almost without exception, parents recalled (with rancor) that once the diagnosis of RLF was made, a chill in relationships developed. At the very time when they needed support and advice, their physicians became distant and defensive, the parents recalled. Most blamed their doctors for failing to maintain interest and concern, not for the failure of clairvoyance! The parents said it was anger at personal, not professional, behavior of physicians, which prompted many of the RLF legal suits charging malpractice which burgeoned in this country.
There is no accurate method of estimating the total number of malpractice law suits, alleging improper use of oxygen, which have been initiated since the 1950s. Some of the actions have been launched when the affected are in their twenties. (This is made possible by the fact that the statute of limitations is reckoned from the time of attaining the legal age of majority; the periods vary from state to state.) There are no satisfactory national statistics which total the decisions reached in legal actions; some have been settled out of court, others have been tried and the opinions are unreported. Several leaders in the blind community have told me that one must not minimize the disservice to the blind which has resulted from these law suits and the publicity announcing enormous awards of money. The actions run counter to the course of the changing status of the blind in our society. There is a move from dependence toward independence and the young adults are ready to demonstrate that their visual loss need not be handicapping if they are given an opportunity to demonstrate their competence. The huge sympathy awards perpetuate the tin-cup stereotype which they wish to erase. If a fraction of the time and money spent in legal battles over RLF were channeled into efforts to provide meaningful employment for blind young hopefuls (physicians and lawyers should be leading the way) our national guilt would be harnessed effectively. Most parents are bitter about the unfair barriers to employment which are being encountered by their children.
I found the discussions with parents extremely disturbing. The problems associated with visual disability seemed minor compared to the endless struggles with members of the helping professions, teachers, and schools (parents fought for years and finally were successful-because of the large numbers of RLF-blinded children-in bringing about a shift in school placement from segregation in residential schools to integration with sighted schoolmates). I was acutely aware of the fact that these interviews with a selected group of parents who had coped successfully could never provide an accurate picture of the full range and incidence of social problems (e.g., abandonment, child abuse, divorce, suicide) associated with the largest oubreak of blindness in American history. The opportunity to obtain reliable information (which would have been useful in developing social support for affected families) was missed in the 1950s.
I do not wish to give the impression that it would have been a simple matter to mount a multidisciplined, long-term study of this complex disorder (which I now envision with the wisdom of hindsight). I must emphasize, however, that this was an early example of the disparity between community need and the pattern of clinical investigation. A high-priority question for the community was, What are the social consequences of RLF-blindness? But, it was a low-priority question for medical inquiry (and the question was never addressed in a systematic fashion). This kind of divergence (not exclusive to medicine) provoked a perceptive editorial by Commoner under the heading “The Responsibility of Science.” He suggested that the disparities arise in a number of ways, some of which have little to do with intellectual challenge (popularly viewed as the motivational stimulus for research). There is a tendency to shun slow-paced, but socially important, studies, he noted, given the present criteria for accomplishment in science: economic support and academic acclaim depend on a high volume of production of publications. His point must not be ignored in debates about the level of public funding for medical studies. I believe that the disincentives of the reward system in clinical research (particularly economic pressure for quick results) did play a role in discouraging organized study of the social consequences of RLF. And it goes a long way in explaining why information concerning the social costs of perinatal rescue operations is so incomplete: studies have focused on the outcome status of individuals — survival, neurologic and intellectual status — rather than the outcome in families and communities. A recent prospective study in North Carolina indicates a disturbingly high rate of social chaos in the families of infants discharged from a newborn intensive care unit (the risk of abuse and neglect was eight times higher than the “expected” rate in the state). The need for more long-term sociologic study is obvious.
While many problems which I have reviewed can be blamed on lack of foresight, technical limitations, or ignorance, there also were other unconscionable failures related to “the feebleness of coordination.” For example, with the help of a superb team of technical experts at Babies Hospital, I once reared a premature infant who weighed 800 grams (1 lb 8 oz) at birth. Three months and several tens of thousands of dollars after birth, the infant was sent home to a Harlem flat. Within a week, we heard that the infant died at night when a rat chewed off his nose. This gruesome example of final results in what might be called the destructiveness of thoughtless benevolence recalls Tom Lehrer’s bitter lyric about rocket weaponry:
Once they’re up, who cares where they come down,
That’s not my department, says Wernher von Braun.
Repugnant as it is to say so, this brutally immoral attitude does shed light on an important dichotomy. Unlike the physician with a rescue fantasy, the weaponry specialist makes a clear distinction between technical decisions and value decisions. Brody observed that scientists or clinicians are prone to confuse scientific problems with value problems and try to solve the latter with tools of the former. But what is the role of professional knowledge in human affairs? In a number of ways, Freidson has suggested, medicine offers the best test of the general question of whether the ends of established professions are so beneficent that experts may be given the autonomy to lead all of society to them. In medicine, actions are based on reliable objective evidence and what the profession deems to be good, the public, on the surface, regards as good. However, there lies at the bottom of medicine’s applied efforts, he correctly observes, a moral, rather than an objective, stance. Further, the professionally defined “good” is asserted to be worth the price the patient is asked to pay in relinquishing his independence. But, unless the moral foundation of medicine is identical to that of the community, Freidson concludes, it will serve not the community but itself.
Earlier, I argued that physicians should closely examine the biologic and social consequences of their actions. However, I must emphasize that it is not suggested that increased sensitivity justifies dominance in the realm of values. The role of a perceptive and sympathetic consultant should not be confused with that of a moral arbiter or an agent of social control. A WHO study group has affirmed the information-giving role of physicians (as opposed to a controlling function) when difficult ethical problems arise in the management of newborn infants with multiple congenital defects. They advised that, as a general rule, decisions should be those of the parents. The physician should be concerned with explaining to the parents, as accurately as possible, the consequences of available options, the group urged. Freidson examined the limits of professional authority, and concluded that the professions, no matter how beneficent their intent, have neither the moral right nor the special qualifications to make choices for the individual or for society. Physicians often make the assumption that “Medical Practice” (especially when it is based on scientifically sound principles) is a pure, moral, acultural phenomenon. I believe that it is this issue-the conflict between the value judgments of doctors and individual families-which has been a major difficulty in the development of perinatal medicine. The clash was discussed at a conference entitled, “Values Underlying the New Childbirth Technology” in 1977.• Participants from a number of disciplines (including child development, economics, history, midwifery, obstetrics, pediatrics, philosophy and policy planning) uncovered many deviations in outlook based on the degree to which pregnancy and childbirth were seen primarily as medical events, or psychological and social events which occasionally require medical assistance. When parent and physician differ in pregnancy and childbirth, who should make decisions concerning care?, was one of the numerous questions debated. Peter Steinfels argued that childbirth, and pregnancy as well, have been transformed into a “medical model” and pregnant women have been assigned a “sick role.” This modern shift has a number of debatable consequences: it mobilizes the coercive power of labels (the terms “low risk” and “high risk” have become judgmental, like “good” and “bad,” “legal” and “illegal”); it shifts authority to the physician and the setting to the hospital; it casts the pregnant patient in a passive role and minimizes her sense of responsibility; and, finally, it justifies the use of specialized, technical, and often very expensive approaches and treatments. As a result, he noted, the childbirth experience has been isolated from other realms of meaning. It has become primarily a medical event rather than a family event, a religious event, or a special moment in the life cycle. This cogent analysis met with vigorous opposition from the medical conferees who argued for a continuation of professional control. The debates served to underline the wide divergence of views among the learned disciplines and the genuine difference in fundamental values among Americans.
I suggest that as knowledge concerning the fetus and newborn has deepened, the profession has sallied forth from the laboratories carrying “truth” on a banner with the same missionary spirit which guided the New England clerics when they invaded Tikopia with Godly truth and stamped out the Melanesian population-control practice of infanticide. But, the frantic evangelism of modern perinatal medicine is puzzling. Given the dismal record of hasty, unevaluated actions in the past, one may very properly ask: What in God’s name is the hurry? One possible answer is provided by historians who have reviewed the Puritan outlook on science and medicine. Webster detects an underlying millenarianism: an attempt to return to the pure state of Adam before the Fall, when man had insight into all truth and power over the created world; when this is achieved the millenium is to be at hand. The evangelist’s drive and hurry to achieve the millenium should be obvious to anyone who looks at the record of the medical science effort of the past few decades. And the quasi-religious fervor has been characteristic of the growth of technology in general. Mumford notes that the demands of mechanical progress have had the effect of a divine ordinance, sacrilegious to challenge, impossible to disobey.
Medicine’s imperative resembles that of fundamentalist religions; the similarity emerges when its value-system clashes with other fundamentalist groups. The Jehovah’s Witness faith, for example, interprets biblical passages from Genesis (“Only flesh with its soul — its blood-you must not eat.”) and from Leviticus (“. . . the soul of every sort of flesh is its blood. Anyone eating it will be cut off.”) as a proscription against blood transfusions. When parents of a newborn infant refuse to consent to an exchange blood transfusion on the grounds of religious freedom, doctors have appealed (successfully) to the courts for permission. This dilemma is usually argued in terms of the limits of the rights of parenthood, but, I suggest, it points up the issue of conflicting value judgements. And, it poses questions concerning the limits of the rights of the dominant culture in a plural society to impose its values on a minority. Brody notes that ethics involves choosing among options which are probability estimates on possible future states, by a process of weighing them against a set of values. The Witnesses keep their eyes on the future prize of everlasting life and they choose not to evoke God’s wrath by breaking His law to extend their lives for only a temporary period of time through blood transfusions. Their children, whose lives have been prolonged (“saved” is a term used in medical fundamentalism) by exchange transfusion, grow up with the belief that they alone, among their co-religionists, have been denied eternal life. These unhappy results of medicine’s self-righteousness recall one of George Bernard Shaw’s maxims for revolutionists, “Do not do unto others as you would that they should do unto you. Their tastes may not be the same. “
The problem of whether moral principles are absolute or relative is an ancient theme in ethics. As I reflect on the dismal results of the moral stands about which I once felt so certain, I find myself siding with those who argue that there is no ethical principle that is acknowledged by all human societies. And I am more willing than ever to accept the view that morals are socially agreed upon values relating to conduct. To this extent morals (and all group values) are the products of social interaction as embodied in culture. These interpretations emphasize that an individual’s or group’s conceptions of what is and what ought to be are intimately connected. And, it follows that the evaluation of risk versus benefit in all medical interventions, proven and experimental, is a highly difficult and individualized process in a multicultural society like the United States.
It has been particularly hard to make value judgments concerning experiments involving human beings. For example, Beecher, in 1966, described 50 clinical studies which he believed violated ethical standards. He arbitrarily selected the intent of the experimenter as the axis of categorization, not the observed risk. This approach has been widely accepted in the past decade. Beecher’s classes have been summarized into two mutually exclusive categories: “therapeutic” and “nontherapeutic” research. But does it fit the real world in which the line between “therapy” and “nontherapy” can rarely be drawn? In addition to philosophic vagaries, placebo-reactor effects blur such neat categorizations. And, more disturbing, this blurring gives rise to deliberate evasions when “nontherapeutic” research is proscribed. Beecher’s dichotomous view of the world of clinical studies is held by many physicians. It is a hold-over from medicine’s past which was ruled by authoritative judgments rather than critical rationalism. The two-value orientation clashes with the scientific view of the world which is probabilistic: judgments are tentative and based on a shifting body of evidence; classifications tend to be scalar rather than categorical. In my opinion, medicine is in the midst of an identity crisis, as it struggles to become scientific. And, I believe, the ambiguity has much to do with the Babel-like atmosphere prevailing in various public forums which have been convened in recent years to discuss the subject of experimentation involving helpless subjects.
Medicine’s slow and uneven shift from mystical certainty to scientific uncertainty has led to a gap in communication between the profession and the community. I suspect there is a feeling of betrayal and confusion at this turn of events. Doctors are viewed suspiciously when they ask questions — a switch from their accustomed role as providers of answers. For example, the Vivisection Investigation League sent out a flier damning controlled experiments on the effects of temperature in premature infants (Fig. 12-3). The writer of the brochure completely misunderstood the question which was addressed by the study and his statements were misleading. In fact, the temperature trial compared survival among infants reared under the standard warming method (used in this country for many years) with the outcome under a new method which kept infants warmer. Survival in the first days of life was improved under the new conditions. Moreover, the question Should newborn babies be kept warm?, turned out to be more complicated than it appeared to the League. Subsequent studies demonstrated that the advantage was temporary. When the warmer conditions were maintained for more than a week, the babies had decreased cold resistance; if inadvertently exposed to the cold during bathing or feeding, they had a diminished capacity to prevent a fall in body temperature.
Public unease with a medical profession that asks questions has also been reflected in the relationships with legislators. One example may illustrate the disturbing consequences of the climate of mistrust. In 1967, a New York State senator created headlines in New York City’s tabloid, The Daily News, with a claim that inhuman experiments in children were being conducted in New York City Municipal Hospitals. He drafted legislation to outlaw all experimentation in children. Deans of medical schools in the state formed an ad hoc group to lobby against the proposed action. This group asked Doctors Joseph Dancis, Lawrence Finberg, and me to draft a white paper on the subject. We prepared a document which advised that the usual defensive posture of academic medicine should be abandoned in favor of a positive approach to deal with the real and unsolved problems. We noted that there was substance to the charge that clinical investigation was conducted more among the poor than among those on higher rungs of the socioeconomic ladder, and that informed consent for studies of the young and helpless was an unsolved problem. We proposed that there should be legislation in the form of an enabling law to encourage properly safeguarded clinical studies involving children, and that a permanent Commission be formed to work on the problem of finding acceptable solutions to the ongoing impediments to proper, scientifically rigorous studies in children.
The senator’s threat was sufficiently grave to cause the president of the Society for Pediatric Research to devote his address to the subject of experimentation in children at the annual meeting of that group in the spring of 1967. The Society’s leader concluded by announcing a Joint Committee on Clinical Investigation in Children which he would chair. Additional representatives from the American Pediatric Society, National Institute of Child Health and Human Development, National Association of Pediatric Department Chairmen and the American Academy of Pediatrics were appointed, I among them. But the committee never met! The senator dropped his attack and the proposed legislation the moment he lost the headlines. And we dropped our responsibility the minute the threat to business-as-usual was removed. Eight years later, I reviewed this episode with one of the principals, and we both agreed that we erred in following legal advice to “lay low.” Subsequent events and the present-day situation indicate how wrong we were not to pursue this matter in a responsible way in 1967. We differed about a judgment concerning additional forces at work. I insisted that the threats to the flow of money for research were met with hasty efforts to sweep all of the untidy bits and pieces under the rug out of view.
The 1967 alarm had the effect of encouraging “bootleg” studies which fall somewhere between the kind of informal studies which I have described in Chapter 10 and formal planned trials. Disguised experiments are those in which research-oriented physicians consciously undertake a series of steps into the unknown without a formal plan or formal peer review. Arguing that bold new treatments are not experimental, but merely “modification or evolution of existing practice” and “based on sound physiologic principles,” they proceed to treat a group of patients. Sticky issues of informed consent and strict review are simply side-stepped. The discipline of the scientific method is ignored in these trials. An example (and it is not unusual) is a study which began early in 1969. A newborn premature infant with severe respiratory distress was treated with a technique (continuous positive airway pressure) which had never been used before in newborn infants. The state of oxygenation in the blood of this infant improved; oxygen concentration in the inspired air was lowered and the seriously ill infant survived. Signed parental consent was not obtained for this new treatment. Contrary to the rules for experimentation involving human subjects which were circulated by the National Institutes of Health in 1966, signed permission was not obtained before the new treatment was applied to 19 more patients with severe respiratory distress. A formal protocol of study was not drawn up or reviewed by a Committee for Human Investigation. There were no randomly assigned concurrent controls who received the standard accepted treatment. Despite all of these violations of the letter and the spirit of the rules governing scientific human experimentation, the study was accepted for presentation at the annual meeting of the Society for Pediatric Research in 1970. Subsequently, the results were accepted for publication by reviewers and editors of the prestigious New England Journal of Medicine.
There have been surprisingly few objections to this kind of poor clinical science that led to the RLF epidemic and to the other catastrophes I have cataloged in Chapter 10. On the contrary, the “Russian roulette” strategy has been condoned and widely praised. Responsible efforts to conduct randomized clinical trials of proclaimed treatments have been characterized as “daring.” One commentator wrote:
While controlled trials are always comforting, it’s probably not a very effective way to assess therapy which may be dependent on a number of variables.
As one attempts to summarize the disharmonies which have accompanied the unprecedented advances in biomedical knowledge in recent years, one point stands out: there is a rift in communications between the medical profession and the community. Physicians have one foot in the empirical past, the other in the new age of scientific inquiry. An ambivalent profession has failed to send out a clear message: early bedside applications are always a leap into the dark. The tedious approach of controls and replications used to reduce the risk of errors in preclinical investigations is needed even more at the clinical step where the complexity and heterogeneity of the interconnected “systems” increase abruptly. In the face of this increased uncertainty, the need for the cautious, hedging discipline of the scientific method increases correspondingly. In the United States there are conflicting attitudes and interests concerning the formats to be used in guiding the application of new knowledge, and all of the clashes are intensified if children are involved. Physicians, who should be in the forefront explaining the principles of the scientific method to parents, politicians, lawyers, etc., are themselves largely alienated from the discipline of planned clinical investigations. But the problem has been growing for some time. It was recognized by Claude Bernard more than 100 years ago when he wrote:
Many physicians attack experimentation on human beings believing that medicine should be a science of observation, but physicians make therapeutic experiments daily on their patients, so this inconsistency cannot stand careful thought. Medicine is by its nature an experimental science, but must apply the experimental method systematically.
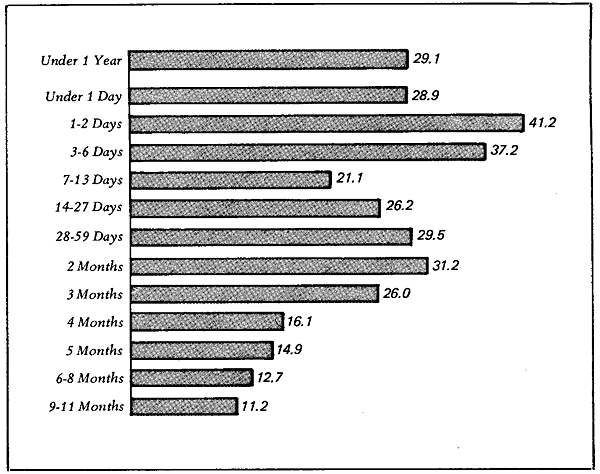
Percent excess of male over female mortality rates by age in the United States (1959-1961).

Mortality by birthweight in the two sexes in the United States (Jan.-Mar., 1950). Deaths under 28 days of age.

Flier circulated by Vivisection Investigation League-Antivivisection Society of New York in the 1960s.
Last Updated on 02/28/24