Retrolental Fibroplasia: A Modern Parable – Chapter 7
Chapter 7
Oxygen Treatment Practices in Premature Infant Care
The practice of administering supplemental oxygen to premature infants began many years before the onset of the RLF epidemic. Inadequate oxygen supply to the tissues is one of the most frequent and most ominous complications in prematurely born infants. This grave difficulty was obvious, even to the unaided eye of caretakers in the past, because of the dramatic color change of the skin from a healthy pink to a sickly blue hue, the color of insufficiently oxygenated arterial blood. This symptom, cyanosis, may be caused by a number of lifethreatening disorders of vital organs (especially lungs and heart), but also occurs in association with inexplicable episodes of cessation of breathing in otherwise normal premature infants.
Budin, in 1900, recommended oxygen inhalation for cyanotic episodes in premature infants. In 1917, Ylppö advised that oxygen be introduced into the stomach by tube as a means of resuscitating premature infants and to manage apnea (arrested breathing). The method was used widely in Scandanavia and in England for many years. In 1922, Hess noted a method, described in 1912, of injecting oxygen under the skin for asphyxial (suffocation) attacks in infants, but he rejected this approach. He recommended, instead, that “The oxygen tank should be kept at the side of the infant’s bed and either continuous or intermittent showers of oxygen given in the attempt to ward off cyanotic attacks.” In 1923, Bakwin studied cyanotic attacks in premature infants and demonstrated that these could be relieved by oxygen inhalations. He noted that when oxygen was administered early, subsequent cyanotic attacks were fewer in number and more readily amenable to treatment. To reap full benefit from treatment, Bakwin recommended that oxygen be given over a long period of time, preferably in a closed chamber.
Hess described an infant oxygen unit, which was used in the Sarah Morris Premature Infant Station beginning in 1931 (Fig. 7-1), in which 346 of 792 infants admitted to the nursery over a three-year period were placed. The indications for treatment were suffocation after resuscitation of the newborn infant, cyanosis, and various lung infections. Oxygen was administered for more than 24 hours, and occasionally as long as 6 weeks. Concentration of oxygen (predicted from flow meter settings, see chapter notes) was usually “40 percent”; in a few instances this was increased to “50-55 percent.” The oxygen policies were credited, in part, for improved survival (Table 7-1).
Table 7-1
Survival of Premature Infants Before and After Infant
Oxygen Unit, Sarah Morris Premature Infant Station, Chicago
| Years | Number of Infants Admitted | Number Which Survived | Survival (%) |
| Before oxygen unit: | |||
| 1922-1926 | 266 | 138 | 52 |
| 1927-1929 | 495 | 335 | 68 |
| After oxygen unit: | |||
| 1931-1933 | 792 | 628 | 79 |
As noted in Chapter 2, skilled, highly opinionated nurses dominated the scene in hospital nurseries before the 1940s. Physicians played a minor role; they entered the nurseries for brief periods, wrote fairly general orders for care, and trusted the specialized nurses to make detailed minute-by-minute decisions concerning clinical management. In the use of supplemental oxygen as a life-saving measure for premature infants, the opinions of “old hands” carried considerable weight. Nurses’ opinions were translated into practice for most of the 70 or so years during which oxygen had been available in hospitals.
Opinion/practice in the matter of oxygen treatment of premature infants can be divided into fairly distinct epochs. In the first period, it was the conventional wisdom that supplemental oxygen improved chances for survival of infants with “asphyxial attacks.” This opinion was led by Madame Louise Recht, the Budin-trained nurse who traveled widely in the United States during the years 1903-1950 (Chapter 2), and Miss Evelyn Lundeen, the dean of American newborn-nursing experts who was Doctor Hess’ head nurse for many years. They firmly supported the view that oxygen treatments were life-saving. Their indications for oxygen were cyanosis and other fairly obvious manifestations of lack.
The second period of oxygen opinion/practice began with observations made in Detroit at the Children’s Hospital of Michigan in 1942. Attention was directed to (1) subtle indicators of the need for supplemental oxygen, and (2) the effects of high concentration of the gas. The breathing characteristics of 33 healthy premature infants were recorded while breathing room air. Of these, 25 breathed in a well-recognized regular-irregular pattern known as “periodic breathing.” when 28 of these asymptomatic infants were placed in a 70-percent oxygen atmosphere, 23 shifted to a regular type of breathing (Fig. 7-2). The authors concluded that
We have no proof that the regular type of respiration which we are accustomed to consider “normal” is “better” for a premature infant than the periodic breathing described. Likewise, we have no convincing evidence that an increased oxygen content of arterial blood is beneficial or necessarily of importance. It is evident, however, that these healthy premature infants breathed in a more normal manner in an oxygen enriched atmosphere.
Also in 1942, Smith and Kaplan reported that the color of the skin in the premature infant was often an unreliable indicator of the state of oxygenation of the blood. Twenty-three premature infants studied between birth and 26 days of life had oxygen saturation levels in blood which were lower than those found in adults or in full-term infants of comparable age; the relatively low levels were not accompanied by a visible blue tinge of the skin. They suggested that the premature infant may be in a state of “subcyanotic anoxia” (oxygen-lack without the tell-tale sign of blue skin color, perhaps as the result of the fact that blood in the capillaries of the skin receives some oxygen directly from the surrounding air by diffusion through the thin epidermis). These observations provided a rationale for the administration of oxygen to asymptomatic premature infants to reduce the risk of brain damage caused by unrecognized oxygen lack.
At the end of World War 11, incubators were designed and built to meet the new specifications of physicians for high-oxygen-concentration capability and improved visibility in the incubator to permit direct observation of the breathing characteristics of premature infants. The Isolette, developed by engineers of the newly formed Air-Shields Company, was the predecessor of the new generation of infant incubators (Fig. 7-3). It was adapted from the design of Chapple, which called for a tightly gasketed chamber ventilated with large volumes of air drawn by a circulating fan from out-of-hospital (or filtered nursery) air to assure outflow of air, thus barring the entrance of nursery air through access ports. This design effectively isolated the infant from airborne contamination, but it did create a problem when high concentrations of oxygen were ordered; dilution of the administered gas with outside air would require a very large oxygen flow to raise oxygen concentration. A rectangular plenum (Fig. 7-4) was designed to solve this technical problem. When outside air was used alone, it was sucked through a screen filter; the air then proceeded through the blower into the heating chamber of the incubator. A cylinder-shaped space above an oxygen nipple housed a small two-tiered float, weighted and designed so that when oxygen was used the flow of this gas raised the float-valve, gradually restricting the intake of outside air. Under these conditions oxygen concentration rose rapidly and permitted efficient use of the expensive gas.
On the day the results of the Cooperative Study were made known to the Air-Shields Company, the president sent a memorandum to every hospital in the world which used the Isolette incubator; it read, in part,
Recommendation — removal of the small float in the air-oxygen intake assembly.
In February 1955, the New York State Health Department mailed an information memorandum on RLF to all health officers, chiefs of medical staffs and hospital administrators in the state (excluding New York City). The bulletin called attention to published articles and editorials implicating oxygen treatment and announced a forthcoming publication which would discuss the control of oxygen therapy to premature infants. The Health Department document noted that “Blindness due to retrolental fibroplasia appears to be entirely preventable . . . If oxygen is administered to premature infants (when clinically indicated rather than routinely), concentrations should be kept below 40%.” The promised article appeared in May 1955; in it, Doctor Lanman of Bellevue Hospital advised that “Oxygen therapy should be given only to infants with clinical signs of respiratory distress and then for as short a time as possible. Concentration should never exceed 40 percent oxygen.” Soon similar advice was given in bulletins, memoranda, and regulations of Health Departments in states and cities throughout the country.
Apart from reasonable doubt about such black-and-white precision on strictly biologic grounds, these statements and recommendations were surprising in view of evidence which had already been made available in the Cooperative Study. As described (Chapter 6) it had been shown that (1) RLF did occur in infants assigned to curtailed oxygen (Table 6-1), and (2) there was no threshold concentration of oxygen which delineated the risk of developing RLF. A later paper from Bellevue, entitled “The Possibility of Total Elimination of Retrolental Fibroplasia by Oxygen Restriction,” again advised that oxygen concentrations only under 40 percent be used. Then Kinsey wrote a letter to the editor objecting to the emphasis which was being placed on the concentration of oxygen:
I have learned that a number of pediatricians have gained the impression that there is appreciably less risk of developing RLF if oxygen is administered at less than 40% concentration . . . In view of the paucity of evidence that there is any critical concentration below which RLF is markedly reduced in incidence, I believe that merely restricting the concentration of oxygen without stringently reducing the duration in oxygen, may result in unnecessary cases of RLF. Certainly the emphasis should be placed on restricting duration in oxygen to an absolute minimum consistent with clinical indications of anoxia irrespective of the concentration of oxygen administered.
Harry Gordon was also prompted to comment on the issue of oxygen restriction. He pointed out that the conclusions of the Cooperative Study concerning the relation of oxygen restriction to the survival rate of premature infants presented a problem:
In the [Cooperative Study] report, it is pointed out that infants were admitted to the study only if they survived 48 hours, and that the mortality figures refer to infants who had already survived the first 2 days of life [italics added] . . . Since the risk of dying from anoxia [oxygen lack] is greatest for premature infants during the first 48 hours, it is obvious that a conclusion such as the one stated (limitation is without an effect on survival] may be misleading.
These warnings by Kinsey and by Gordon went largely unheeded. An epoch of oxygen opinion/practice, which may be called the “under-40%-era,” was ushered in at the end of 1954. Concentrations of oxygen administered to premature infants were carefully monitored by serial measurements in the incubators and so long as the concentration remained below 40 percent, many felt secure that the infant was safely and properly protected from the risk of RLF.

Fig. 7-1. Hess bed equipped with an oxygen therapy unit (A-side and B-top views). 1.-Pressure gauge, 2.–oxygen flow regulator, 3.-flow meter 4.-glass and metal hinged door for feeding purposes, 5.-thermometer window, 6.-metal hinged door for purposes of body care of the infant, 7.-ventilator with small and large exit openings, 8- 12. – controls for maintaining temperature in water-jacket of the incubator.
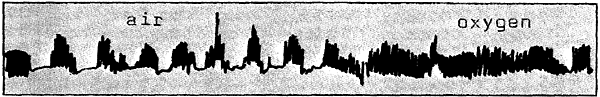
Breathing patterns of a healthy, small premature infant. A “periodic” pattern in room air, “regular” in 70-percent oxygen.

A pre-1954 individually ventilated Chapple-type incubator (blow-up view). Air was drawn into the incubator at the rate of 10 liters per minute to prevent the accumulation of carbon dioxide produced by the infant occupant and to bar the entrance of nursery air when the access ports were opened to care for the infant. The plexiglass hood made the respiratory movements of the naked infant in the incubator highly visible to attendants. *See details of air-oxygen intake block in Fig. 7-4.

Air-oxygen intake assembly of the pre-1954 model Isolette incubator. A two-tiered float valve was raised by the flow of oxygen to restrict the flow of diluting outside air into the incubator.
Last Updated on 02/28/24