Fetal Monitoring
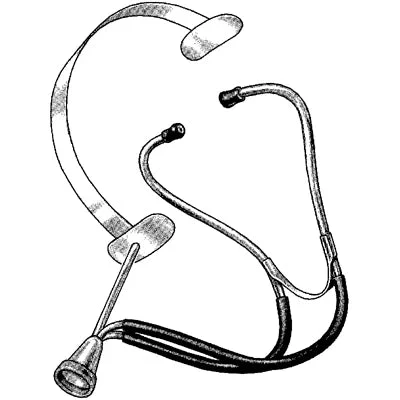
The concept that fetal heart rate could reflect fetal well-being dates to the 1600s, with Marsac credited with the first detection of fetal heart sounds and Killian with the first proposal of their clinical significance. Practical auscultation entered obstetric practice in 1818 when Mayor and Kergaradec described placing the ear against the maternal abdomen, and by 1833 Evory Kennedy had published formal guidelines for its use in intrapartum monitoring. The Pinard horn — a simple acoustic stethoscope — became the standard tool from the mid-19th century onward, while Von Winkel’s 1893 criteria for fetal distress (tachycardia above 160, bradycardia below 100, irregular rhythm, meconium, and altered fetal movement) defined the clinical threshold for concern and went essentially unchanged for the next 70 years.

The first significant instrument advance over simple ear-to-abdomen auscultation came in 1917, when David Hillis at the Chicago Lying-In Hospital described a fetal stethoscope purpose-built for intrapartum monitoring. In 1922, his superior at the same institution, Joseph DeLee, described the device independently — generating lasting controversy over priority — and it eventually entered practice as the DeLee-Hillis fetoscope, remaining the dominant tool for intrapartum surveillance for the next half-century. DeLee himself advocated a structured auscultation regimen: every 30 minutes during the first stage of labor, and every three to five minutes — or continuously — during the second stage, with any of Von Winkel’s established signs of fetal distress taken as an indication for forceps delivery. By the 1940s, amplified electric fetoscopes developed by Matthews, Marvel, and Kirschbaum made the task easier still, and intermittent auscultation (IA) consolidated its place as the emerging standard of care, a position it held well into the 1970s and that persists in modified form today.
Meanwhile, parallel efforts to extract more objective information from the fetal heart signal were producing mixed results. Cremer’s 1906 description of fetal ECG acquisition via abdominal and intravaginal leads prompted a generation of investigators to pursue electrocardiographic markers of fetal distress — an effort ultimately abandoned when no consistent ECG pattern could be identified. Henly’s 1931 description of electronic phonocardiography, which simply used a microphone to amplify auscultated heart sounds, was a more modest advance in the same direction. Neither approach solved the underlying problem of continuous, reliable fetal surveillance, but both kept the concept alive and pointed toward the electronic solutions that would follow in the 1950s.
The transformation of fetal surveillance from intermittent auscultation to continuous electronic monitoring emerged from parallel and largely independent lines of research on three continents during the 1950s and early 1960s.
In Uruguay, Roberto Caldeyro-Barcia and his colleague Hermógenes Alvarez began by tackling the problem of quantifying uterine activity. Working at the University of Montevideo, they recorded intrauterine pressure by placing balloons inside the uterus, developing what became known as Montevideo units — a measure of the cumulative force of contractions during labor. By 1958, they had extended this work to demonstrate the effect of uterine contractions on fetal heart rate, defining normal and abnormal fetal responses through continuous monitoring. The characteristic abnormal response — a heart rate fall following the contraction peak — they called “type II DIP,” a pattern that would later be renamed late deceleration by others working in the field.
That same year, working independently at Yale, Edward Hon published the first description of a system for continuously capturing the fetal ECG electronically. Where Caldeyro-Barcia had approached the problem from the physiology of uterine contractility, Hon brought a background in electronics — he had trained at the Marconi School of Wireless in Sydney before pursuing medicine — to the problem of signal acquisition. His system enabled obstetricians to track fetal heart rate continuously through contractions and to measure contraction strength and frequency simultaneously, providing a real-time window into fetal tolerance of labor. Over the following decade, Hon systematically correlated specific heart rate patterns with fetal acid-base status, defining the clinical significance of early, late, and variable decelerations and establishing the interpretive framework that underpins EFM classification to this day.
In Germany, Konrad Hammacher (1928-2001) approached the engineering challenges of reliable signal capture, pioneering methods to reduce noise-to-signal ratios in fetal heart rate recording. In 1962 he published a new method for selective registration of the fetal heartbeat, and in 1966 he proposed that oxytocin-induced contractions in late pregnancy could be used to predict fetal tolerance of labor — a concept that became the basis of the contraction stress test.
Hammacher’s collaboration with Hewlett-Packard’s Böblingen division ultimately produced the HP 8020A in 1968, the world’s first commercially available non-invasive fetal monitor and the device that brought cardiotocography into clinical practice at scale. Though it was originally available in 1968 only in the European market, around 1970 it became the first major Hewlett-Packard product to be imported to the United States after being developed overseas.
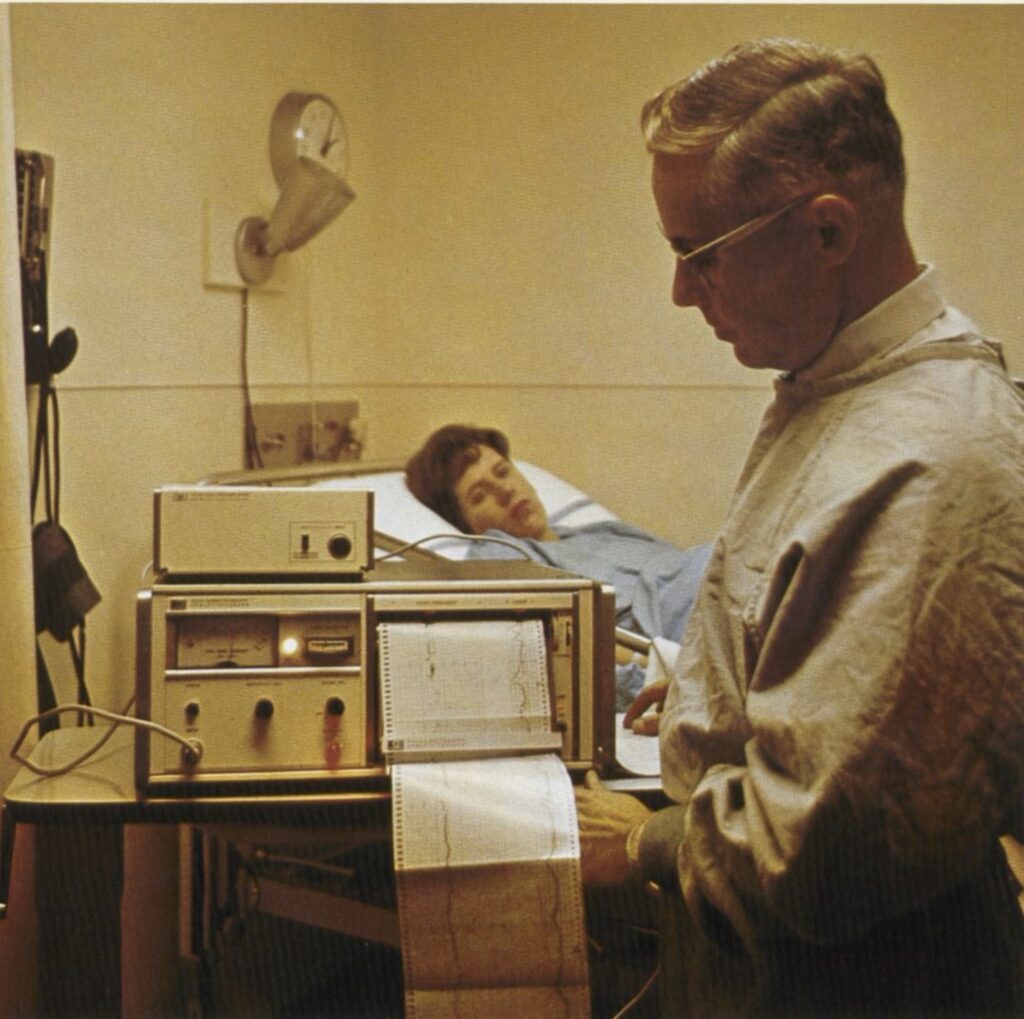
Continuous electronic fetal heart rate monitoring was introduced into hospitals in the 1970s without evidence from clinical trials, with a strong marketing push from the monitoring industry. The machine was marketed as a scientific breakthrough that could predict fetal distress and end cerebral palsy. From introduction of the first commercial monitor in 1968 to 1976, a survey found most obstetric residency programs used EFM; by 1979, at least one-half of all laboring women were monitored electronically.The pervasive use of continuous fetal monitoring has become controversial, critics say that it dramatically increases Cesarean section rates without reducing cerebral palsy or neonatal death.
As EFM expanded into antenatal care, early observers recognized that the fetal heart rate record carried prognostic value even without contractions — specifically, the acceleration of heart rate with fetal movement — and this became the basis of the nonstress test (NST). Frank Manning and colleagues formalized antepartum surveillance further in the early 1980s with the biophysical profile (BPP), which combined five fetal variables (heart rate reactivity, breathing movements, gross body movement, tone, and amniotic fluid volume) into a composite score, improving predictive accuracy beyond any single test.
Decades of inconsistent terminology — more than eight competing nomenclature systems published between 1975 and 1995 — hampered both research and clinical communication. In response, the NICHD convened expert panels in 1995–96 and again in 2008, with Julian T. Parer (UCSF) instrumental in leading the first workshop. The resulting 1997 report established standardized definitions for baseline rate, variability, accelerations, and deceleration types, while the 2008 workshop — co-sponsored by ACOG and the Society for Maternal-Fetal Medicine — added the three-tier classification system (Category I normal, Category II indeterminate, Category III abnormal) that became the U.S. standard. In 2015, a 50-expert FIGO international consensus endorsed “cardiotocography” (CTG) as the preferred global term for the combined monitoring of fetal heart rate and uterine activity.
Key Milestones in Fetal Monitoring
| Year | Event |
|---|---|
| 1818 | Mayor and Kergaradec describe fetal auscultation |
| 1833 | Kennedy publishes fetal distress auscultation guidelines |
| 1893 | Von Winkel establishes criteria for fetal distress |
| 1906 | Cremer describes fetal ECG acquisition |
| 1947–1950 | Caldeyro-Barcia and Alvarez develop intrauterine pressure recording; Montevideo units described |
| 1958 | Hon publishes first continuous electronic FHR capture; Caldeyro-Barcia correlates uterine contractions with FHR changes |
| 1962 | Hammacher publishes selective FHR registration method |
| 1968 | HP 8020A — first commercial fetal monitor released |
| 1972 | Hon introduces the fetal scalp spiral electrode |
| Early 1980s | Manning develops biophysical profile scoring |
| 1997 | NICHD Research Planning Workshop establishes standardized FHR terminology |
| 2008 | NICHD second workshop; three-tier classification system adopted by ACOG |
| 2015 | FIGO international consensus; “cardiotocography” endorsed as preferred global term |
- History of Fetal Monitoring. https://ob-efm.com/efm-basics/history/
- Ayres-de-Campos D. “Electronic fetal monitoring or cardiotocography, 50 years later: what’s in a name?” Am J Obstet Gynecol 2018;219(1):6–8. DOI: 10.1016/j.ajog.2018.03.011.
- “The Worst Test in Medicine” – New York Times
Last Updated on 04/02/26