Louise Amélie Leonie Recht (1872-1951)
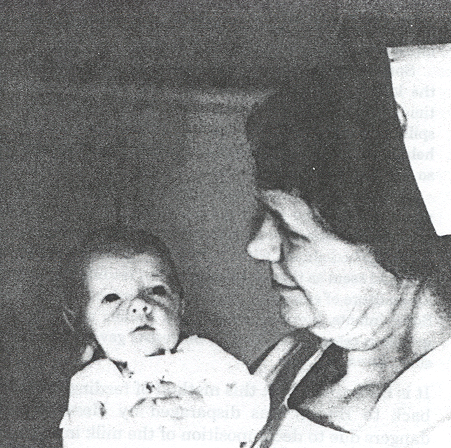
Few figures in the early history of neonatal care are as consequential—or as underrecognized—as Amélie Louise Recht, a French nurse whose career spanned five decades and two continents. Born on August 15, 1872 in Chilly Mazarin, France, and trained at the birthplace of modern premature infant medicine, she carried the clinical methods of the Paris Maternité across Europe and eventually to the boardwalks of America, serving as the indispensable human link between the hospital-based innovations of the 1890s and the formative premature infant stations of the twentieth century. Her work with premature infants is documented in contemporary accounts over a 46 year period, from 1897 to 1943.
The Paris Maternité at Port-Royal was, in the final decades of the nineteenth century, the most important center for obstetric innovation in the Western world. It was here that Étienne Stéphane Tarnier, the hospital’s chief obstetrician, introduced the first practical infant warming device — a double-walled wooden box with a glass lid and a water reservoir heated by a gas burner — in 1880, after observing a chicken-egg incubator at the Paris Zoo. Within three years, Tarnier had documented a marked reduction in mortality among premature infants weighing less than 2,000 grams who were cared for in his couveuses.
A special ward for sick and premature newborns — the Pavillon des Enfants Débiles, or “weaklings’ pavilion” — was established at the Maternité in late 1893 under the direction of Madame Henry, Tarnier’s Midwife-in-Chief. The pavilion housed up to twelve incubators and established nursing routines that were, by the standards of the time, remarkably systematic: infants were weighed before and after each feeding, human milk was delivered by breast, by spoon, or by gavage tube into the stomach, and wet nurses were required to wash and gown themselves before approaching the babies. When Tarnier retired in 1895, he was succeeded as head of the Maternité by his former student Pierre-Constant Budin, who expanded the premature infant unit, systematized feeding protocols, and became the most influential figure in European neonatal medicine.
It was in this environment that Louise Recht received her training. The historical record does not preserve the exact dates of her education or the details of her early life, but by 1897 she was sufficiently accomplished to be named in the British medical journal The Lancet by her professional title — Mdlle. — and identified as having been “specially trained at the Paris Maternity Hospital to look after debilitated and prematurely born infants reared in incubators,” in a special service that admitted some 400 children annually born under the most unfavourable circumstances. Although no documentation of her training at the Maternité has been discovered to date, there is plenty of concrete evidence of her skills acquired there.
It appears that Madame Recht was drawn into Martin Couney’s orbit through her friendship with Solomon Fischel. (The October 20, 1913 New York Times story about Fischel’s sudden death in 1913 states “One of Dr. Fischel’s associates of long standing was Madam Louise Recht, who came from Paris with him in 1900…”) Couney and Samuel Schenkein, a businessman and promoter, were inspired by the success of the “Kinder Brutanstalt” at the Berlin Exhibition of 1896 to put on a similar incubator incubator exhibit at the Victorian Era Exposition of 1898. The British hospital system declined to lend him premature infants for display, so Couney obtained babies from Paris instead. There is no evidence that Couney trained under Budin or had any connection with Budin (despite his claims), so it seems likely that Fischel’s friendship with Recht was the connection used to source these babies. Recht then assisted Couney and Schenkein with the management of the incubator exhibit until it closed.
Madame Recht arrived in the United States at Ellis Island aboard La Gascogne on April 27, 1903 (passenger ID 102638030262). She gave her destination to immigration as “Mr. Schenkein at the Fulton Building,” but apparently she moved in with the Couneys immediately or shortly after her arrival. Her co-residence with the Couney family is documented in the 1920 and 1940 US Censuses. Martin Couney cosigned her petition for citizenship, and she was naturalized and took the oath of allegiance in New York on August 21, 1924. A. J. Liebling, writing in The New Yorker in 1939, described her household status plainly: “Madame Louise Recht, the head nurse, a Frenchwoman who has been Dr. Couney’s chief aide for forty-one years and always lives with the Couneys, has an adjoining room and bath.”
Recht became a permanent fixture of Couney’s Coney Island operation after it opened at Luna Park in 1903. Inside the exhibit, the atmosphere was — whatever the barkers outside might have suggested — strictly professional. At peak operation, the nursing staff included fifteen trained nurses working in eight-hour shifts and five wet nurses providing human milk. Recht is also remembered for a signature gesture with visitors: Madame Recht occasionally wowed the crowds with a special trick — placing her diamond ring around a baby’s wrist to show the public how small the infants truly were. This trick has apparently become part of neonatology folklore, to the point where my own neonatology attending when I was a fellow would sometimes demonstrate it to parents of extremely small premies.
More significantly, Recht maintained the French nursing protocols she had learned at the Maternité: meticulous weight recording, scheduled feedings, strict hygiene, and gavage feeding for infants too weak to suckle. These were not theatrical props but genuine clinical methods. She also managed the nursing side of the enterprise during one of its most dangerous moments: in August 1917, a Luna Park ride called the toboggan burst into flames, next door to the incubators. Recht, Fischel, another nurse, and a couple of policemen, carried all 11 babies to safety.
The most enduring legacy of Louise Recht’s career is the knowledge she transmitted to the first generation of American hospital-based neonatal nurses. The central conduit was Evelyn Lundeen, the head nurse of the Premature Infant Station that Dr. Julius Hess established at the Sarah Morris Children’s Hospital within Chicago’s Michael Reese Hospital in 1922 — the first premature infant station in the United States, recognizing the importance of nursing care and temperature management in the care of preterm babies.
Recht taught Lundeen the French techniques of gavage feeding and nasal feeding. Gavage feeding became the standard premature infant-feeding technique. The nasal feeding technique was never recorded in Hess’s books, apparently because Lundeen did not believe that it worked or was safe. Nasal feeding is documented, however, in a film made in 1939 at Couney’s New York World’s Fair exhibit, in which Recht is shown using a teaspoon with upturned edges to pour small quantities of milk into the nose of a premature infant who swallowed it without difficulty.
Lundeen went on to build the Michael Reese premature station into a national model. She traveled extensively to teach other nurses about the care of preterm babies, and historians credit Lundeen with shaping the role of nurses in neonatal care. She and Hess co-authored The Premature Infant: Its Medical and Nursing Care (1941, revised 1949). By World War II, health departments in more than two dozen states had established premature infant care programs, most following the “Chicago model” Lundeen and Hess had pioneered. At the foundation of that model were practices Louise Recht had carried from the Paris Maternité to Earl’s Court to Coney Island to Chicago.
Louise Recht’s career is a study in how clinical knowledge travels through institutional gaps. In an era when hospital medicine largely declined to care systematically for premature infants, dismissing them as “weaklings” with poor survival prospects, it was a trained nurse who preserved and transmitted the most advanced practices of French neonatal nursing across nearly half a century of commercial exhibition. She was not the originator of the techniques she taught; those belonged to Tarnier, Budin, and the nursing culture of the Paris Maternité. But she was their carrier, and without her presence at Couney’s side from 1897 to 1943, the chain of transmission from Paris to Chicago might have broken entirely.
Although the roles of nurses are often not as visible in written history as the men who held power at the time, evidence suggests that the quality care administered by nursing staff was a key factor in the greater survival rates experienced by premature infants in their care. Recht is perhaps the clearest example of this pattern in the early history of neonatology. Her name appears in the primary sources with some variation — Mademoiselle Recht in the 1897 Lancet, Madame Recht in later accounts, Aunt Louise to those who knew her — and her full given name, Amélie Louise Leonie Recht, appears in only a handful of records. She outlived all of the Couneys except Hildegarde; her date of death is documented as April 15, 1951 in the New York State death register and the Brooklyn Eagle (April 16, 1951, page 9), and Dawn Raffel was able to find her headstone. What is better documented is her presence across more than forty years of an enterprise that saved thousands of infants who had no other recourse.
- Raffel, Dawn. The Strange Case of Dr. Couney: How a Mysterious European Showman Saved Thousands of American Babies. New York: Blue Rider Press, 2018. The most thorough modern biography of Couney; documents Recht’s April 27, 1903 arrival aboard La Gascogne (Ellis Island Passenger ID 102638030262) and Schenkein’s payment of her passage. Available via Amazon.
- Silverman, W.A. “Incubator-Baby Side Shows.” Pediatrics 64 (August 1979): 127–141. Foundational historical account; the first scholarly work to bring Recht’s role into focus. Available at https://neonatology.net/history/classic-books/incubator-baby-sideshows-silverman/.
- Prescott, S., and Adriance, V. “Premature Infant Care in the Early 20th Century.” Newborn & Infant Nursing Reviews 17, no. 2 (2017): 56–61. Peer-reviewed nursing history article examining the contributions of Recht and Lundeen. Abstract via ScienceDirect.
- Liebling, A.J. “Patron of the Premies.” The New Yorker, June 3, 1939. The most detailed contemporary description of Recht’s daily life and role. Available at https://neonatology.net/history/classic-books/4719-2/.
- Editors, The Lancet. “The Victorian Era Exhibition at Earl’s Court.” July 17, 1897. Original source identifying Recht by name and professional training. https://neonatology.net/history/classic-books/4705-2/
- NIH Symposium: “Neonatal Intensive Care: A History of Excellence.” 1985. Contains a detailed account of the Recht–Lundeen knowledge transfer. neonatology.net/pdf/nic.nih1985.pdf.
- Ellis Island Arrival
- Naturalization Petition
- Oath of Allegiance
- US Census 1920
- US Census 1940
- Death Notice – Brooklyn Eagle, April 16, 1951
Last Updated on 04/22/26